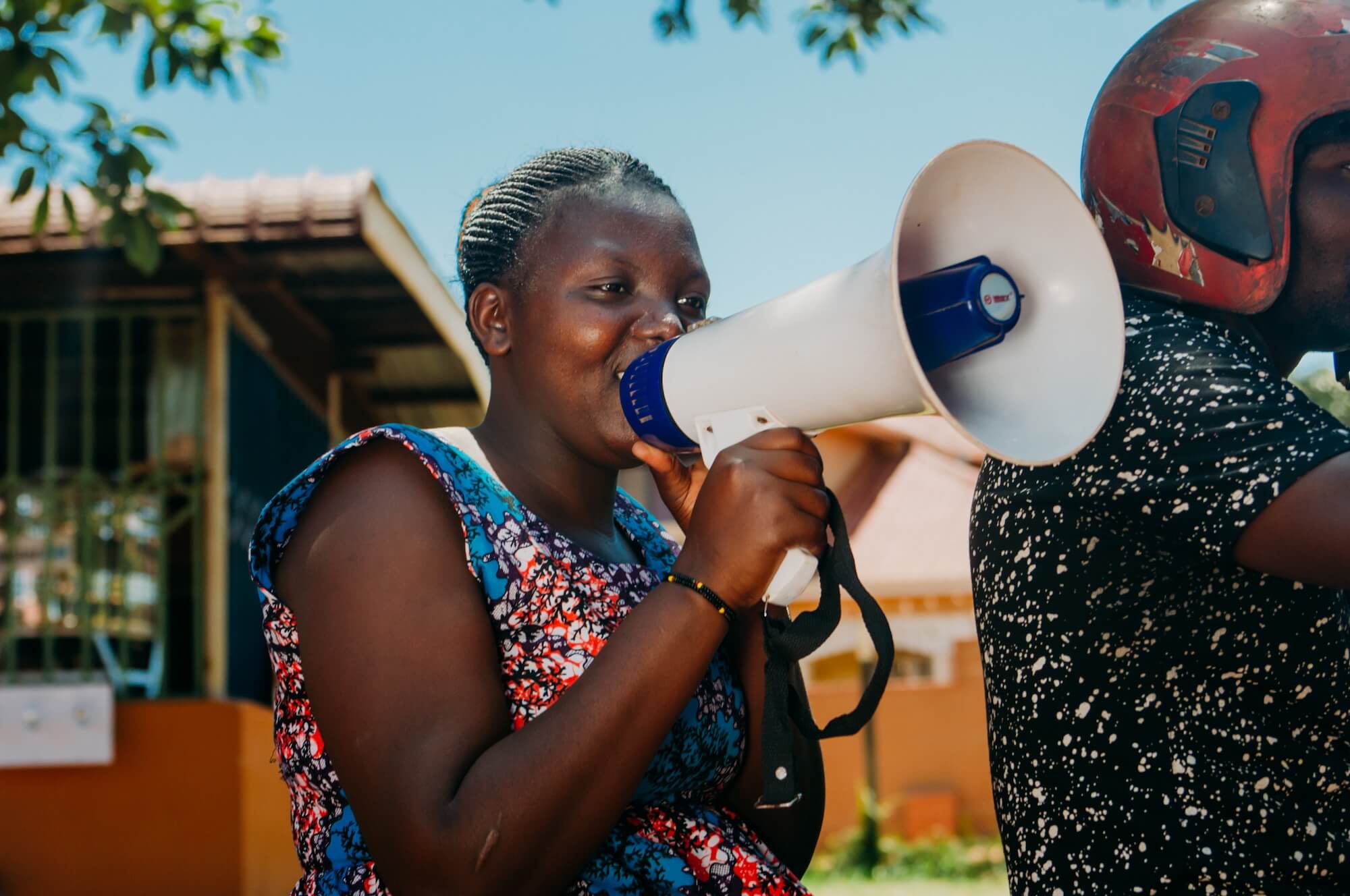Our providers continue to show courage and determination in the face of adversity.
We are in the midst of a global pandemic and the world is turned on its head. The emergency facing us is becoming increasingly uncertain and more and more countries around the world face restrictions and national lockdowns.
Many of our programmes and team members around the world have been affected by the crisis and are working hard to ensure they can keep delivering for the women and girls who need them, while keeping our clients and team members safe.
Madagascar
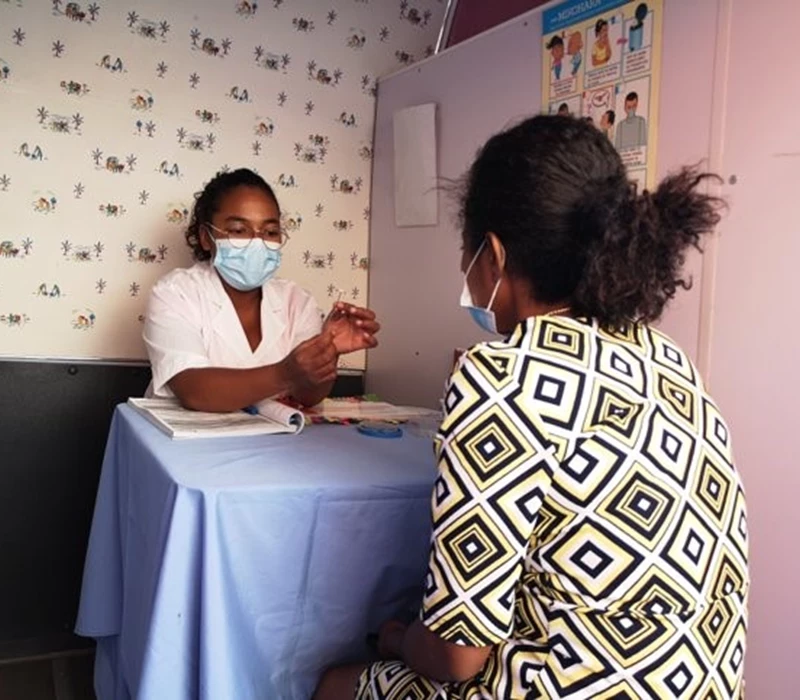
With lockdowns leading to curfews, transport blocks, and the cancellation of market days, which would usually provide a cover for women wanting to access services discreetly, many women have been unable to reach facilities. In Madagascar, for example, travel restrictions meant women were unable to access maternity hospitals, post-abortion care or contraceptive services.
However, our teams have adapted their methods in order to continue to serve women. Our team in Madagascar accessed government permits for our MSI buses to be allowed on the roads. This meant that our services could be delivered directly to women in their homes, or that women could be safely transported to health facilities without fear that they would be turned back at transport blocks.
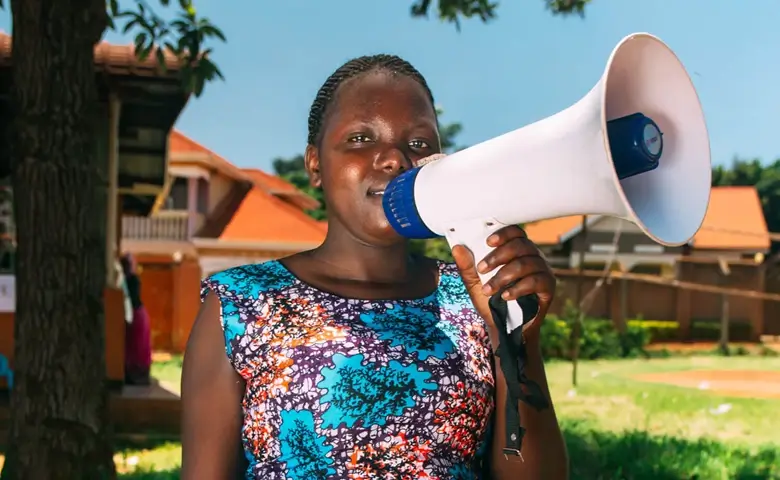
Uganda
On the 20th March, the Government in Uganda responded to the COVID-19 pandemic by imposing a lockdown restricting travel across the country. These restrictions varied between districts, with some imposing stricter and more aggressive penalties than others.
When it became clear that these travel restrictions prevented women from accessing sexual and reproductive health services, the MSI team set up a pilot project, in partnership with UNFPA, to deliver healthcare products using the SafeBoda ride-hailing mobile app. The project allows women to order reproductive health commodities, including condoms, contraceptive pills, emergency contraception, pregnancy test kits, HIV testing kits, and menstrual health products, through the e-Shop, and an MSI Lady packs the products and gives them to a boda boda rider, who then delivers the products directly. The service has allowed women in the Kampala and Wakiso districts to order and receive reproductive health commodities at their doorsteps and has the potential to be scaled up across more districts in Uganda.
Mali
As some women are cautious of visiting health facilities during during the pandemic, our programmes have worked to build community awareness around our commitment to COVID-19 prevention. For example, our programme in Mali conducted a major awareness campaign, both to build public awareness around COVID-19 risks and of the measures the programme is taking to protect clients.
Through radio shows, Facebook broadcasts and community-based campaigns, the team were able to ensure that their local communities felt comfortable accessing MSI’s services and were armed with accurate information on how to guard against infection.

“We try to adapt our strategies to serve our sisters, our daughters in their time of need. It’s a great source of motivation for us, and makes us forget about the virus a little. Together, we will overcome the challenges facing us – we’ll do whatever remains possible!”
Team member in Mali
Sierra Leone
We know that in previous health crises diverting resources away from reproductive healthcare can lead to additional deaths. During the Ebola epidemic, as many, if not more people died in Sierra Leone from increased barriers to maternal and reproductive healthcare than from the virus itself.
“The [Ebola] crisis led to a spike in the number of teenage pregnancies. People were too afraid to go to hospital or government facilities. If we had stopped providing contraception and post-abortion care, it would have been much worse… People will always need services, irrespective of an epidemic.”
Felix Ikenna, Dr and Quality Assurance Director, MSI in Sierra Leone
Understandably, the government were keen to prevent a repeat of the spike in teenage pregnancies seen during the Ebola crisis, so immediately involved MSI. The Ministries of Education and Gender collaborated with us at district level and through emergency committees to focus on contraceptive access for young people, while publicising sexual health advice and information on youth services via school radio programmes.


Bengaly, MSI Lady in Burkina Faso
Bengaly, a midwife and MSI Lady in Burkina Faso, is adapting to new challenges in order to continue to provide care to the women and girls who need her. She is able to navigate through quarantines and roadblocks by using her excellent relationships with local healthcare providers who help coordinate her visits, and even uses the quarantine checkpoints as an opportunity to educate the officers in sexual and reproductive health when travelling between villages.
To ensure the safety of herself and her clients, she has implemented the latest guidance to minimise the risk of COVID-19 infection, for example, by ensuring social distancing in the waiting areas. Her commitment has meant that she is able to continue to deliver essential contraceptive services to the women in her community. Because, as she says, “even in the most difficult situations, we have to be able to meet the needs of our clients”.
United Kingdom
As soon as the UK went into lockdown on March 23rd, MSI Reproductive Choices UK began advocating passionately for the introduction of telemedicine to ensure that women could continue to access the timely, safe and high-quality abortion care they need. Shortly after, in April, we launched a telemedicine service, enabling women to receive tele-consultations and self-administer medical abortion drugs at home.
Since April, our telemedicine programme has provided over 7,000 UK women with medical abortions, and feedback shows that is well-received by both clients and providers, with 98% of clients rating their experience as good (14%) or very good (84%). We are now sharing learnings from our UK programme to explore similar models for remote provision in low resource settings, for example South Africa, India and Nepal.


Zimbabwe
When the government in Zimbabwe announced a nationwide lockdown on 17th March, we heard reports from women seeking our services being turned away by police at roadblocks despite the government having declared SRH essential.
Shortly after, MSI’s programme (PSZ) set up an emergency response team, alongside SIDA Zimbabwe, to deliver services to women in rural areas. They integrated family planning into the local immunisation programme, ensuring rural women could still access services. In just two weeks, they served over 3,500 rural women and girls with family planning.
With support from DFID and SIDA, all services across PSZ’s centres, outreach, and social franchise channels have remained open, which has enabled the programme to reach as many women as possible, despite the number of women able to travel to service-delivery points decreasing.
Nepal
When the government ordered a national lockdown in Nepal, neither providers nor clients were able to reach MSI’s centres, forcing them to close.
But by working in partnership with local government, our team in Nepal were able to ensure women could still access care. They played an active role in a co-ordinated response between government, NGOs and multi-lateral organisations, to ensure continued access to SRHR services, even in the context of a strict lockdown.
As a leading member of the Reproductive Health Sub-Cluster, a multi-stakeholder group led by the Family Welfare Division and UNFPA, MSI Nepal helped influence the swift approval of interim guidelines which were implemented across the country. As well as allowing clients and health workers to have temporary exemptions from COVID-19 travel restrictions, the guidelines allow medical abortion (MA) services to be provided in client’s homes. Trained service providers and volunteers are now allowed to provide door to door delivery of medical abortion drugs and services, and trained chemists can store and distribute MA drugs.


Tika, MSI Lady in Nepal
In the Sindhuli district in Nepal, we find Tika. She is a qualified midwife and a MSI Lady, a collective of midwives and nurses who travel from village to village, door to door to deliver high-quality services to women in their own communities.
Working in remote areas of the country, people often need to walk far to access her services, something that for many has become impossible during the nationally imposed lockdown due to COVID-19. “I am still providing services, but they are limited. People often need to walk far to reach me and the lockdown has meant they are unable to get here.”
Despite the challenges, Tika remains determined to do whatever she can to serve the women in her community. “Today I walked four hours to deliver contraceptive services to a woman who called me asking me to come over… No pandemic should prevent women from accessing sexual and reproductive health services.”

As the world is facing a global emergency, we need your support.
During these difficult times, our ability to continue to serve some of the worlds most vulnerable and marginalised women is becoming increasingly uncertain. With your support, we can continue to do so.
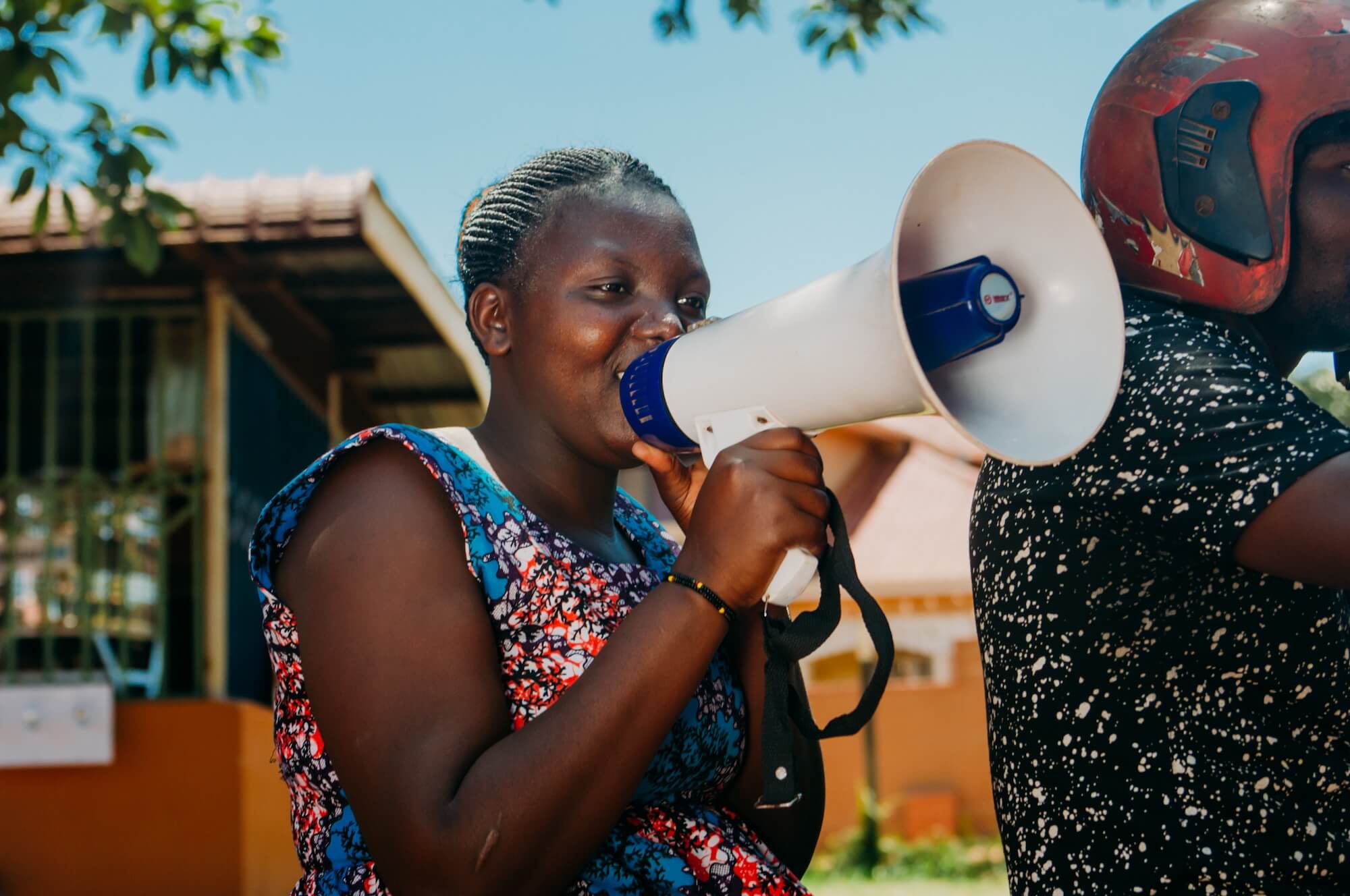
Want to join the movement for reproductive rights?
Sign up to receive the latest news, views, frontline stories, and campaigns on reproductive health and rights, straight to your inbox.